Rabies Exposure and Prevention: Spread and Protection
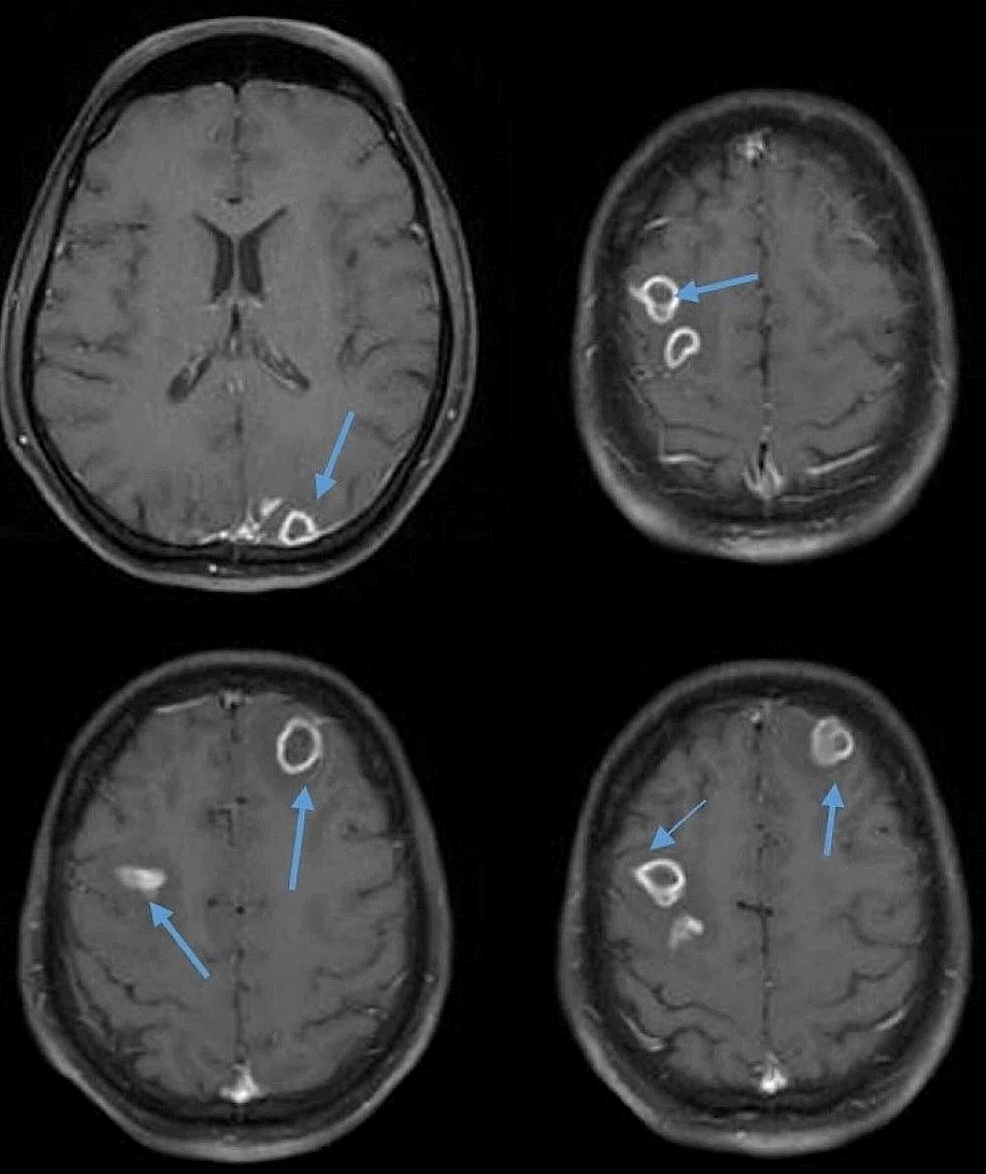
Introduction Rabies exposure and prevention are critical topics for anyone at risk of contact with infected animals. Rabies is a deadly viral disease that attacks the central nervous system and is almost always fatal once symptoms appear. Most human infections occur through bites or scratches from infected mammals, including dogs, bats, raccoons, and other wildlife. Despite being preventable through vaccines and timely medical care, rabies continues to claim thousands of lives worldwide each year, particularly in regions with limited awareness or access to healthcare. Understanding rabies exposure and prevention involves knowing how the virus spreads, identifying high-risk situations, and taking immediate action after potential contact with an infected animal. Early intervention, such as wound cleansing and post-exposure prophylaxis, can completely prevent the onset of the disease. Communities, healthcare providers, and individuals all play a key role in reducing rabies-related fatalities through education, vaccination programs, and responsible animal management. This guide explores how rabies spreads, the symptoms that follow exposure, the risk factors in different environments, and the practical prevention strategies that can protect both humans and animals. The goal is to provide actionable, accurate information to minimize risk, encourage timely medical care, and raise public awareness about this deadly yet preventable disease. Understanding Rabies and Its Transmission Rabies is caused by a virus belonging to the Lyssavirus genus, which primarily spreads through the saliva of infected animals. While bites are the most common method of transmission, scratches, open wounds, or contact with mucous membranes—such as the eyes, mouth, or nose—can also lead to infection. Animals that commonly carry rabies include dogs, bats, raccoons, skunks, foxes, and coyotes. Worldwide, unvaccinated dogs remain the leading source of human rabies deaths, while in the United States, exposure to bats accounts for most cases. The virus primarily affects the central nervous system, leading to inflammation in the brain and spinal cord. Once symptoms appear, rabies is almost always fatal, which underscores the importance of early prevention and prompt post-exposure care. Recognizing Rabies Symptoms in Humans Rabies has an incubation period ranging from weeks to months. During this time, infected individuals may experience no symptoms. As the disease progresses, initial signs resemble flu-like symptoms, including fever, headache, fatigue, and general malaise. Discomfort or tingling at the site of exposure is often an early clue. As the virus advances, neurological symptoms emerge, including confusion, anxiety, agitation, hallucinations, and aggressive behavior. A hallmark sign of rabies is hydrophobia, or fear of water, where individuals panic at the sight of fluids despite feeling extreme thirst. Excessive salivation, difficulty swallowing, and muscle spasms may also occur, ultimately leading to death if untreated. Groups at Higher Risk of Rabies Certain populations face an elevated risk of rabies exposure. Travelers to regions with endemic rabies, people who work closely with animals, and those who explore wildlife habitats are particularly vulnerable. Occupations such as veterinarians, wildlife handlers, laboratory researchers working with live virus, and animal control officers are at greater risk and often recommended to undergo preventive vaccination. Preventive Measures Against Rabies Preventing rabies relies on multiple strategies, both for humans and animals. Vaccination remains the cornerstone of prevention. Pets should receive regular rabies vaccinations, and children should be taught not to approach or handle unfamiliar animals. Ensuring bats and other wildlife cannot enter living spaces reduces exposure risks. Pre-exposure vaccination, known as pre-exposure prophylaxis, is recommended for individuals at high risk. This typically involves two doses of the rabies vaccine spaced a week apart, with periodic antibody checks depending on risk level. For the general population in areas with low incidence, pre-exposure vaccination is generally unnecessary, but post-exposure prophylaxis remains essential if exposure occurs. Immediate Actions After Potential Exposure If a person is bitten or comes into contact with a potentially rabid animal, prompt medical attention is critical. The wound should be washed immediately with soap and water, and medical professionals should be contacted to assess the need for rabies immunoglobulin and vaccines. https://www.who.int/teams/control-of-neglected-tropical-diseases/rabies/vaccinations-and-immunization For individuals who have never been vaccinated, both rabies immunoglobulin and a series of vaccines are administered. Those previously vaccinated require additional booster doses without immunoglobulin. Containment or testing of the animal involved, when safely possible, helps determine the appropriate treatment course. Rabies in Animals and Public Health Measures Surveillance and vaccination of animals play a crucial role in reducing human rabies cases. Wildlife management, stray animal control, and public education campaigns contribute to lowering exposure risks. Maintaining rabies-free domestic pets and wildlife vaccination programs in endemic areas has been shown to dramatically reduce human fatalities. Global Perspective on Rabies Rabies remains a major health concern globally, causing an estimated 60,000 deaths annually, with 95% occurring in Africa and Asia. Effective control strategies, including vaccination campaigns, public awareness programs, and robust medical infrastructure, are critical for reducing rabies-related mortality. Conclusion Rabies is a preventable but deadly viral disease. Understanding how it spreads, recognizing symptoms early, and implementing preventive measures are vital for protecting both humans and animals. Vaccination, safe handling of animals, and immediate medical care following Rabies exposure and prevention potential exposure remain the most effective strategies. Public awareness and proactive health measures can dramatically reduce the risk of this fatal disease.