Kissing Bug Disease in the US: Symptoms & Treatment
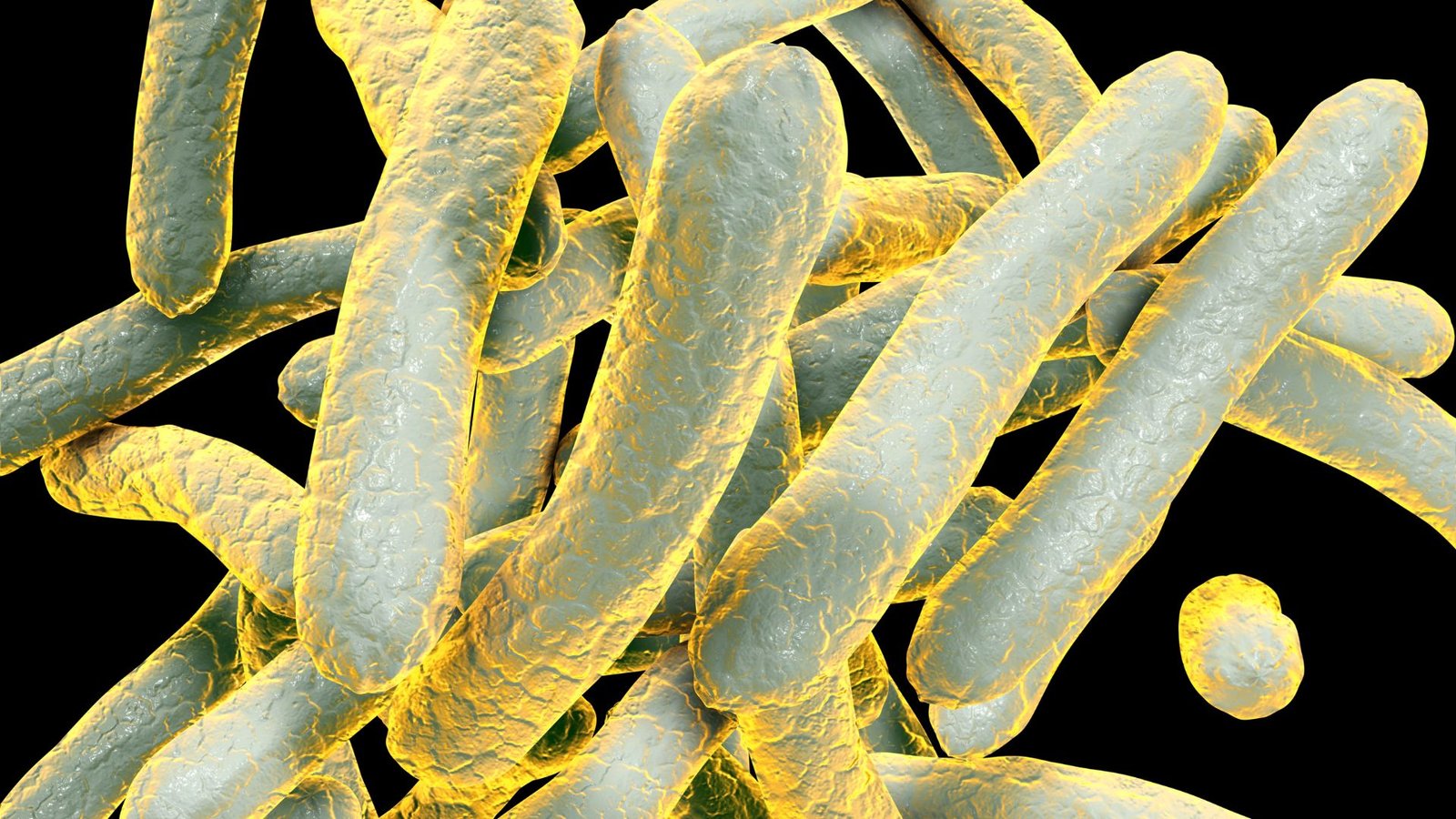
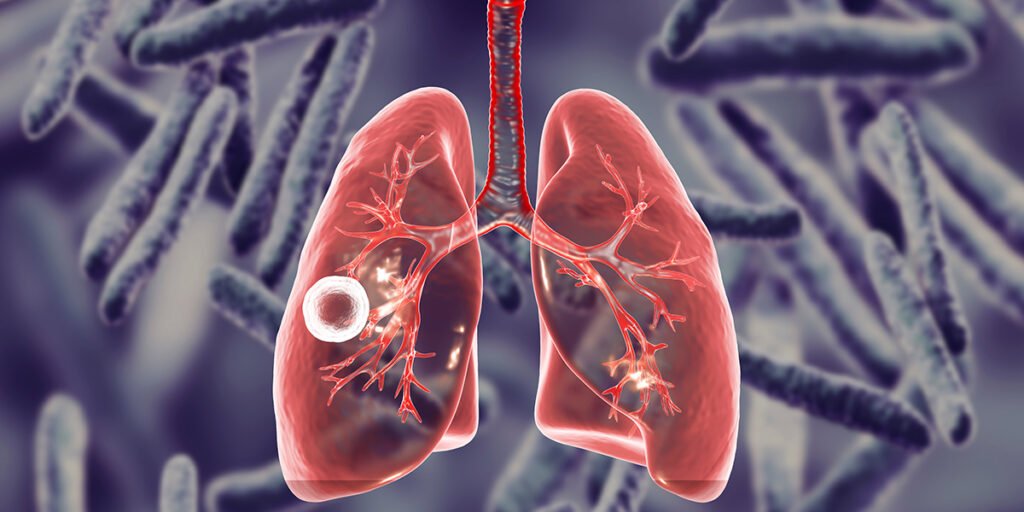
Chagas Disease in the US: Introduction and Overview Kissing bug disease, caused by the parasite Trypanosoma cruzi, is an emerging public health concern in the United States. This disease, also known as Chagas disease, is primarily transmitted by kissing bugs, or triatomines. Once thought to be limited to Latin America, recent research confirms that kissing bug disease now affects several regions across the US. Experts warn that without proper awareness, testing, and preventive measures, many Americans may remain unaware they carry this potentially life-threatening infection. The infection often goes undiagnosed early because initial symptoms are mild or nonspecific. By the time chronic complications, such as serious heart and digestive problems, appear, the disease may have been present for years. Increasing public and medical awareness significantly improves early detection and treatment outcomes. Overview of Kissing Bug Disease Chagas disease is caused by the protozoan parasite Trypanosoma cruzi. The World Health Organization classifies it as a neglected tropical disease, and it is widely established in many Latin American nations. In the United States, it is increasingly considered an emerging health concern, particularly in the southern states where kissing bugs are more common. Causes and Transmission of Kissing Bug Disease In the United States, the most common method of transmission is through the bite of infected kissing bugs. These insects feed at night and often defecate near the bite site. Infection occurs when the parasite in the bug’s feces enters the body through the eyes, mouth, mucous membranes, or broken skin. Transmission can also occur through contaminated blood transfusions, organ transplants from infected donors, congenital transfer from mother to child, and, in rare instances, contaminated food or drink. Many infections progress unnoticed because symptoms in the early stage are minimal. Early Symptoms Chagas disease develops in two distinct stages: acute and chronic. Early Symptoms The acute phase lasts a few weeks to a few months, during which individuals may experience fever, weakness, fatigue, headache, swelling at the site of the bite, rash, nausea, vomiting, or diarrhea. These mild signs often resemble common viral illnesses, making the condition difficult to detect in the early phase. Chronic Complications If the disease remains untreated, it may lead to chronic complications involving the heart, digestive tract, and nervous system. Long-term effects include heart failure, cardiac arrhythmias, enlargement of the esophagus or colon, stroke, and sudden cardiac death. Research indicates that between twenty and thirty percent of infected individuals eventually suffer from serious complications, emphasizing the importance of early diagnosis. Kissing Bugs and Their Spread in the US Kissing bugs are blood-feeding insects commonly found in warmer climates, especially in the southern regions of the United States.https://www.who.int/health-topics/chagas-disease#tab=tab_1 States with Known Kissing Bug Populations Scientists have confirmed the presence of kissing bugs in at least thirty-two states, including Texas, Arizona, California, Louisiana, Florida, Mississippi, and Arkansas. Climate shifts may allow these insects to expand into more northern regions, increasing the risk of transmission in additional areas. Infected Mammals and Pets Research reveals that several animals act as reservoirs for Trypanosoma cruzi. Infected mammals include raccoons, opossums, armadillos, coyotes, and domesticated pets such as cats and dogs. Veterinarians in affected states have reported cases among pets and zoo animals, which shows that the disease extends beyond human populations. Epidemiology of Chagas in the US The Centers for Disease Control and Prevention estimate that around 280,000 people in the United States are currently living with Chagas disease, though the exact number of individuals with chronic complications is uncertain. Human Cases in Kissing Bug Disease Documented human cases have been identified in states such as Arkansas, Arizona, California, Louisiana, Missouri, Mississippi, Tennessee, and Texas. Because Chagas disease is not nationally reportable in most states, a significant number of infections may go undetected. Public Health Implications Acknowledging Chagas disease as endemic in the United States would improve surveillance, enhance public education, increase funding for treatment and research, and prompt healthcare providers to screen at-risk groups more effectively. Many experts believe that viewing Chagas solely as a foreign disease has delayed the development of adequate public health strategies. Diagnosis of Chagas Disease Early detection is essential for successful treatment outcomes. Blood Tests and Screening Diagnosis usually relies on serological tests that detect antibodies against Trypanosoma cruzi. Screening is especially important for individuals who donate blood, pregnant women with potential exposure, and patients with unexplained heart or digestive problems. Challenges in Detection Kissing Bug Disease A major obstacle to timely diagnosis is the limited familiarity of US healthcare professionals with Chagas disease. Many patients only learn of their infection when they donate blood or when chronic complications have already begun. Treatment Options There is currently no vaccine for Chagas disease, but timely medical treatment can be effective, particularly during the early phase. Benznidazole and Nifurtimox The primary treatments are antiparasitic medications such as benznidazole and nifurtimox. These drugs work best during the acute stage, although some individuals in the chronic phase may still benefit from therapy. Managing Long-Term Complications In chronic cases, treatment centers on managing symptoms and preventing progression. Physicians focus on controlling heart failure and arrhythmias, addressing digestive disorders, and monitoring stroke risk. Consistent medical follow-ups and lifestyle adjustments improve the outcome for many patients. Preventing Chagas Disease Prevention focuses on limiting contact with kissing bugs and reducing the possibility of infection. Reducing Contact with Kissing Bugs Preventive actions include sealing cracks and gaps in homes, installing window screens, removing nesting or shelter areas near houses, and keeping pets indoors at night in high-risk locations. Public Health Measures Public health programs in countries where the disease is common have achieved success through community education and vector control efforts. Experts in the United States recommend similar strategies, such as training healthcare providers, launching awareness campaigns, and improving disease surveillance. Expert Insights and Global Comparisons Medical specialists emphasize the importance of recognizing Chagas disease as a domestic health concern. Nations such as Bolivia, Argentina, and Chile have reduced infection rates through coordinated strategies and public health initiatives. In contrast, US prevention efforts remain limited,…