GLP-1 Medication Type1 Diabetes: Risks, Benefits, and Research
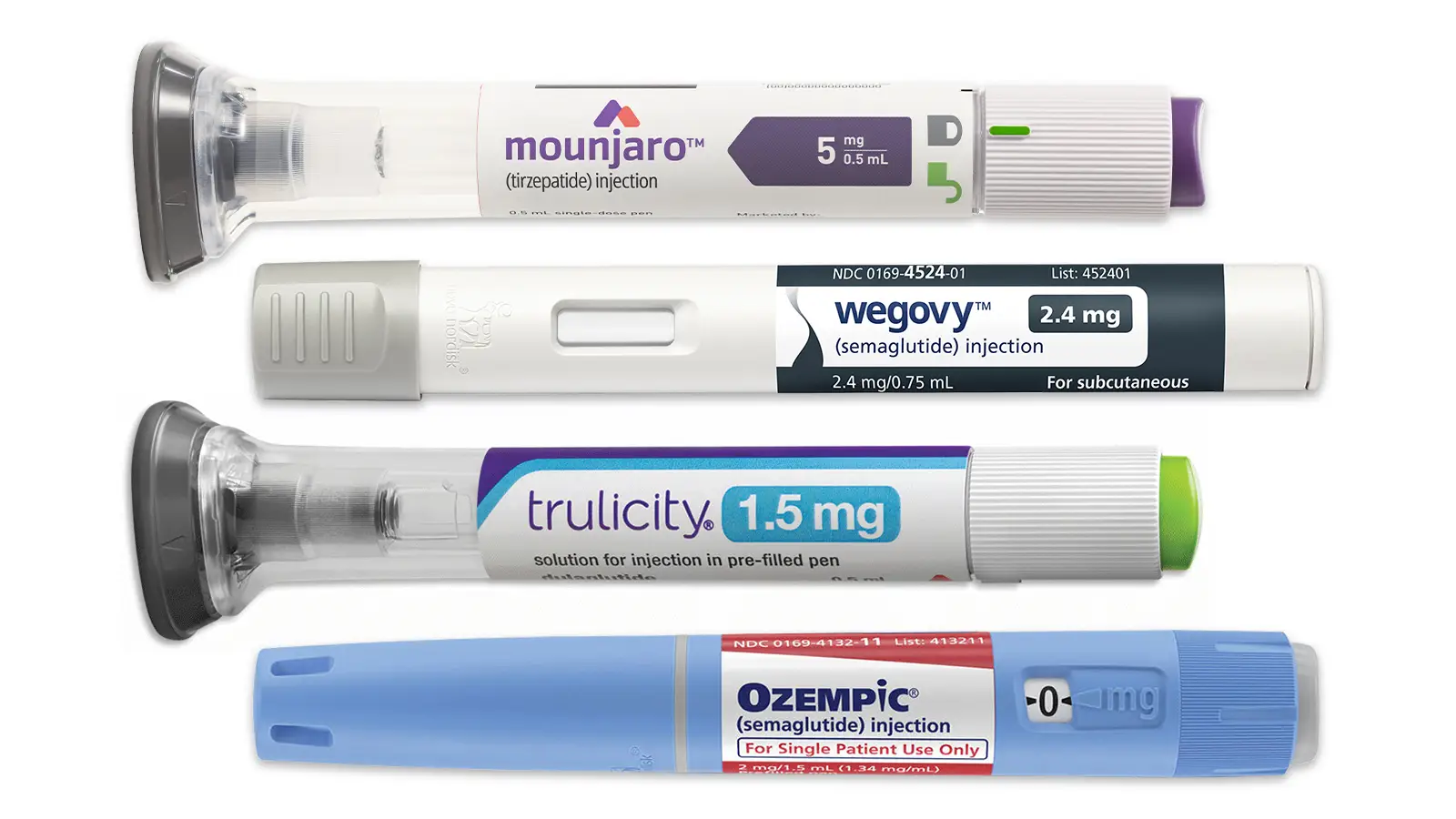
Introduction GLP-1 medication type1 diabetes use has been rising steadily, even though clinical evidence on their safety and effectiveness for people with type 1 diabetes remains limited. Medications like Ozempic, Wegovy, Zepbound, and Mounjaro were originally developed to treat type 2 diabetes, where the body becomes resistant to insulin. These drugs have also shown benefits in promoting weight loss, supporting cardiovascular health, and improving metabolic function in non-diabetic patients. However, individuals with type 1 diabetes depend entirely on insulin because their bodies cannot produce enough on their own. Using GLP-1 receptor agonists alongside insulin has raised concerns about potentially dangerous low blood sugar, and formal studies in type 1 populations are still scarce. Despite this, off-label prescriptions have become common, particularly for patients with type 1 diabetes who struggle with obesity or fluctuating blood sugar levels, highlighting a growing trend in clinical practice. Understanding GLP-1 Medications GLP-1 receptor agonists mimic the body’s natural glucagon-like peptide-1 hormone, which plays a crucial role in regulating blood sugar. These medications stimulate insulin secretion, slow the emptying of the stomach, and increase satiety, making them effective for controlling blood sugar and aiding weight management. Although these drugs have proven safe and effective for type 2 diabetes, their use in type 1 diabetes remains largely unexplored. The potential for low blood sugar and the lack of formal clinical trials in type 1 populations make careful monitoring essential. The Rising Obesity Trend in Type1 Diabetes Obesity rates among people with type 1 diabetes have been increasing over the past decade. Among children aged two to nineteen, obesity has risen from 18% to 26%, while in adults aged twenty and older, it has increased from 30% to 38%. This upward trend in obesity has prompted clinicians to explore additional treatment options, including GLP-1 medications, to help manage weight and improve glycemic control. For type 1 patients, maintaining a healthy weight is particularly challenging because insulin therapy can contribute to fat storage. Use of GLP-1 Medication in Type1 Diabetes Some type 1 diabetes patients report that GLP-1 medications help stabilize their blood sugar, reduce insulin requirements, and support weight loss. These benefits are most pronounced in patients with obesity, who face a higher risk of complications from insulin resistance and metabolic stress. However, not all type 1 patients benefit equally. Those who are not overweight may experience more gastrointestinal side effects, which can lead them to discontinue the medication. Careful dosing and close supervision by an endocrinologist are essential to prevent hypoglycemia, a potentially life-threatening condition that can occur if insulin and GLP-1 medications are not balanced properly. Evidence and Safety of GLP-1 Medication in Type1 Diabetes The current evidence for using GLP-1 medications in type 1 diabetes comes primarily from retrospective and observational studies. These studies suggest that some patients may experience improved blood sugar control and weight loss, particularly those who are insulin-dependent and overweight. Researchers have not conducted enough randomized controlled trials specifically for this population, which makes it difficult to fully assess long-term safety and efficacy. Patients commonly report side effects such as nausea, vomiting, and diarrhea, and hypoglycemia remains a key concern. Ongoing Clinical Trials Several clinical trials are currently investigating GLP-1 medications in type 1 diabetes. One study involves patients using an artificial pancreas system, which automatically adjusts insulin delivery based on continuous glucose monitoring. Researchers give participants weekly injections of semaglutide, a common GLP-1 drug, and monitor them for six months to evaluate blood sugar control, weight management, and safety. Another long-term trial at Yale University will follow patients for a year, with results expected in 2028. These trials aim to provide the rigorous, randomized data necessary to guide safe and effective use of GLP-1 medications in type 1 diabetes. Potential Benefits When prescribed appropriately, GLP-1 medications can help reduce insulin needs in type 1 patients with obesity. They can also stabilize blood sugar levels and support weight loss. Additionally, these drugs may offer cardiovascular benefits, improving lipid profiles and reducing inflammation in other populations. Anecdotal reports suggest better glucose control and improved quality of life. However, comprehensive clinical trials are needed to confirm these effects and ensure long-term safety. Risks and Limitations for GLP-1 Medication in Type1 Diabetes Despite their potential benefits, GLP-1 medications carry significant risks. Hypoglycemia is a primary concern when combined with insulin therapy, particularly for patients with fluctuating blood sugar levels. Gastrointestinal side effects are common and may interfere with adherence. Additionally, long-term effects of these drugs in type 1 diabetes are not well known. Careful monitoring and individualized treatment plans are essential. GLP-1 medications may not be suitable for all type 1 patients. This is especially true for those who are not overweight or have gastrointestinal disorders. Clinical Guidance for Patients Patients considering GLP-1 therapy should work closely with an endocrinologist to determine if the medication is appropriate. Blood sugar should be monitored rigorously, and insulin doses adjusted accordingly. Any adverse effects should be reported immediately.If side effects occur, or the medication is ineffective, other options can be considered. These include dietary changes, more exercise, or SGLT-2 inhibitors. Personalized approaches are critical, as responses to GLP-1 medications can vary widely among type 1 diabetes patients. https://diabetes.org/living-with-diabetes Future Directions The increasing off-label use of GLP-1 medications in type 1 diabetes underscores the urgent need for high-quality clinical trials. Researchers are focusing on identifying patient populations who are most likely to benefit, optimizing dosing strategies, and understanding long-term outcomes. With rigorous scientific evaluation, GLP-1 medications could serve as an important adjunct therapy. They may help manage weight and improve blood sugar control in type 1 diabetes patients, especially those with obesity-related challenges. Conclusion for GLP-1 Medications in Type1 Diabetes GLP-1 medications type 1 diabetes usage is a rapidly evolving area of clinical practice. Preliminary evidence suggests potential benefits for weight management and blood sugar control. However, risks such as hypoglycemia and gastrointestinal side effects require careful monitoring. Ongoing clinical trials will provide essential guidance on the safety and effectiveness of these drugs in type 1 diabetes….