Legionnaires’ Disease: Symptoms, Treatment, and Prevention
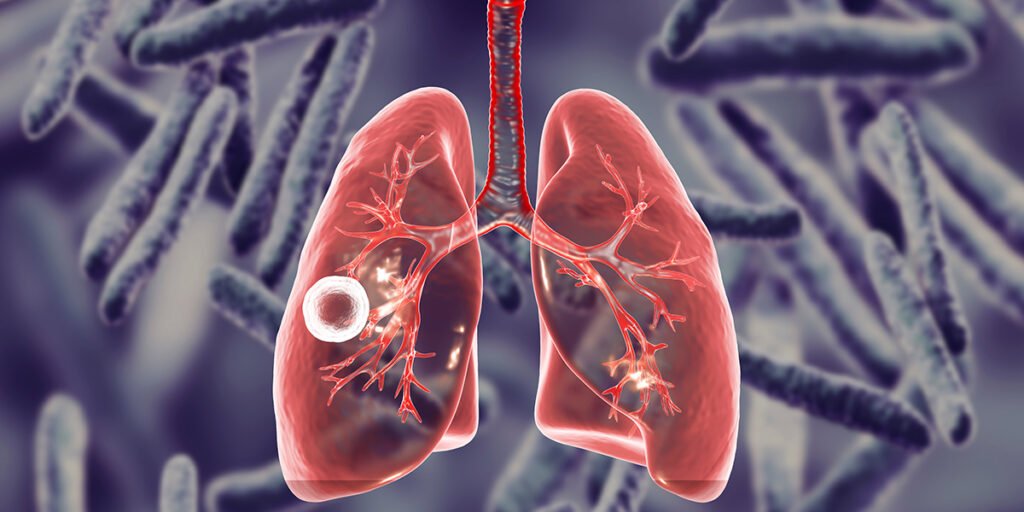
Introduction: Understanding Legionnaires’ Disease Legionnaires’ disease is a severe form of pneumonia caused by the Legionella bacteria. While most people may not be familiar with this infection, it has the potential to cause serious illness and even death if left untreated. Legionnaires’ disease often emerges in clusters, linked to contaminated water or air systems in buildings, making it a critical public health concern. Although the disease can affect anyone, certain populations, such as older adults and people with underlying medical conditions, face a higher risk of developing severe complications. Public awareness, early detection, and preventive measures are essential to controlling outbreaks and safeguarding community health. Causes and Transmission of Legionnaires’ Disease Legionnaires’ disease is caused by Legionella bacteria, which are naturally found in freshwater environments such as lakes, rivers, and soil. The bacteria become a problem when they grow and spread in human-made water systems, such as hot tubs, cooling towers, plumbing systems, and decorative fountains. Humans typically contract the disease by inhaling aerosolized water droplets containing the bacteria or accidentally aspirating contaminated water into their lungs. Unlike many types of pneumonia, Legionnaires’ disease does not spread from person to person. Outbreaks are frequently associated with large buildings or facilities where water systems are not adequately maintained. Historical investigations have shown that hotels, hospitals, cruise ships, and nursing homes are particularly vulnerable to Legionella proliferation if proper disinfection protocols are not in place. Risk Factors for Severe Illness Not everyone exposed to Legionella bacteria will become ill. Individuals with underlying health conditions such as chronic lung disease, kidney disease, diabetes, cancer, or immunodeficiency are at increased risk of severe disease. A history of smoking also raises the likelihood of complications, as does being 50 years or older. Healthy individuals may contract Legionnaires’ disease, but their risk of severe complications is generally lower. Understanding these risk factors helps public health authorities identify vulnerable populations and prioritize preventive interventions. Symptoms and Clinical Presentation Legionnaires’ disease can begin with symptoms that resemble the flu, making early recognition challenging. Common symptoms include cough, high fever, shortness of breath, headaches, and muscle aches. Gastrointestinal symptoms such as diarrhea, nausea, and abdominal pain are also frequent, and some patients experience neurological symptoms, including confusion. Symptoms typically appear within two to 14 days after exposure. Severe complications can develop, particularly in at-risk populations. These complications include respiratory failure requiring mechanical ventilation, kidney failure, septic shock, and multi-organ infection, which can ultimately lead to death. Because of the disease’s severity, timely medical attention and accurate diagnosis are crucial. Pontiac Fever – A Milder Form In addition to Legionnaires’ disease, Legionella bacteria can cause a milder, flu-like illness known as Pontiac fever. While individuals with Pontiac fever generally recover without specific treatment, it serves as a warning sign of Legionella exposure and emphasizes the importance of monitoring water systems to prevent severe outbreaks. Diagnosis of Legionnaires’ Disease Diagnosing Legionnaires’ disease involves a combination of tests. Respiratory specimens, obtained through sputum collection, and urine antigen tests are the primary methods used to detect the presence of Legionella bacteria. Timely diagnosis is essential to initiate effective treatment and prevent complications. Physicians must maintain a high index of suspicion, particularly for patients presenting with pneumonia who have potential exposure to contaminated water sources. Early detection significantly improves the chances of recovery. Treatment Options for Legionnaires’ Disease Antibiotic therapy is the cornerstone of Legionnaires’ disease treatment. Commonly used antibiotics include levofloxacin, azithromycin, doxycycline, and rifampin. The choice of medication depends on factors such as the patient’s overall health, preexisting conditions, and whether the infection was acquired in a hospital or community setting. Supportive care is often required for patients with severe symptoms, including supplemental oxygen or mechanical ventilation. Early intervention reduces the risk of complications and improves survival rates. Preventing Legionnaires’ Disease Prevention strategies focus on reducing the growth and spread of Legionella bacteria in water systems. Proper maintenance of plumbing systems, cooling towers, hot tubs, and decorative fountains is critical. Facilities should implement water management programs that identify potential risks and apply control measures, including regular flushing, disinfection, and temperature monitoring. For individuals, avoiding inhalation of aerosolized water from high-risk sources, such as poorly maintained hot tubs or misting systems, helps reduce the chance of infection. Awareness of environmental sources and symptoms ensures early medical evaluation and reduces the likelihood of severe disease. Cleveland Clinic – Legionnaires’ Disease: Causes, Symptoms & Treatment Public Health Measures Public health authorities play a vital role in preventing Legionnaires’ disease outbreaks. Investigations following reported cases include testing water systems, identifying contamination sources, and ensuring complete disinfection. Regulatory guidelines and monitoring programs for large buildings, hospitals, and other institutions help maintain safe water systems and prevent future outbreaks. Community education on Legionnaires’ disease and its risk factors further strengthens prevention efforts. Outbreak Investigation and Response Effective outbreak management requires rapid detection and response. In past outbreaks, public health departments have traced infections to specific water sources, such as cooling towers in large buildings. Remediation involves thorough cleaning and disinfection to eliminate Legionella bacteria. Follow-up monitoring ensures that preventive measures are effective and that no further cases occur. Long-Term Implications Legionnaires’ disease serves as a reminder of the importance of water safety in public and private facilities. Building managers, healthcare providers, and public health officials must maintain vigilance to reduce the risk of exposure. Proactive water system management, combined with early medical recognition of symptoms, can prevent fatalities and limit the public health impact of Legionella bacteria. Conclusion Legionnaires’ disease is a serious and potentially deadly infection that requires awareness, prevention, and timely treatment. Understanding the causes, symptoms, risk factors, and preventive measures is critical for individuals, healthcare providers, and public health authorities. Proper maintenance of water systems, early diagnosis, and effective treatment are key strategies for reducing the impact of this disease. By remaining informed and proactive, communities can minimize the risk of Legionnaires’ disease and protect public health.