Viral Infections Increase Heart Attack Risk, Study Finds
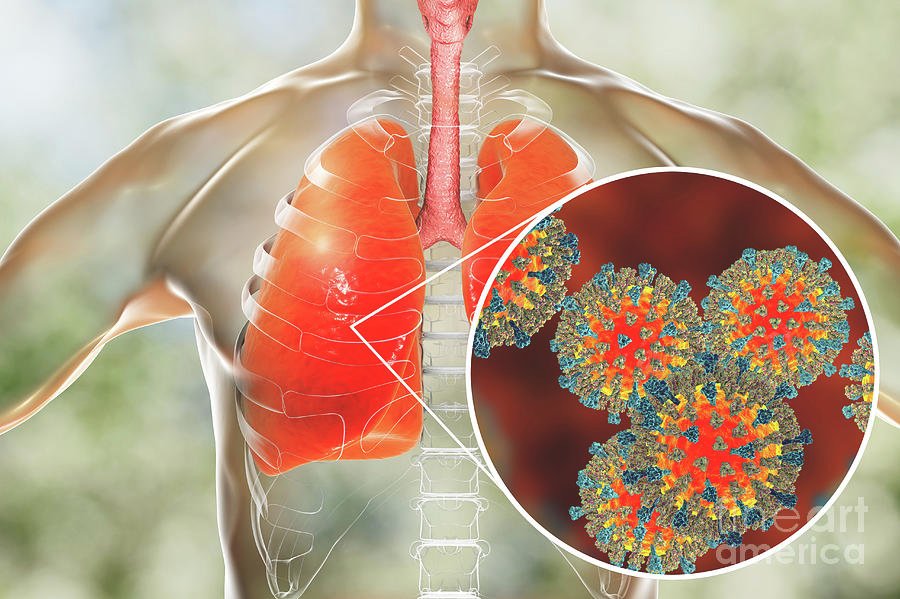
The Alarming Link Between Viruses and Cardiovascular Health Viral infections increase heart attack risk, according to new research that sheds light on how common illnesses may affect long-term heart health. For decades, medical science has recognized that infections can have far-reaching consequences beyond their immediate symptoms. However, recent studies have revealed a troubling connection between viral infections and cardiovascular disease. A comprehensive meta-analysis published in the Journal of the American Heart Association has confirmed that common viral illnesses such as influenza, COVID-19, HIV, hepatitis C, and shingles can heighten the risk of heart attacks, strokes, and other serious cardiovascular complications. The research analyzed 155 studies spanning several decades, using global data to explore how viruses influence the cardiovascular system in both the short and long term. According to the findings, individuals who contract the flu are up to six times more likely to experience a heart attack within the month following infection. Similarly, those who have suffered from COVID-19 face nearly double the risk of developing cardiovascular complications compared to those who have not been infected. Lead author Dr. Kosuke Kawai, adjunct professor at the David Geffen School of Medicine at UCLA, emphasized that vaccination offers a dual advantage — not only preventing infection but potentially safeguarding heart health as well. “Often, we get vaccinated to reduce the risk of influenza or other illnesses, but vaccines can provide an additional benefit in terms of protecting against cardiovascular disease,” he noted. The Science Behind Viral Infections and Heart Disease The association between viral infections and heart disease is complex but biologically plausible. When a virus enters the body, the immune system activates an inflammatory response to fight off the infection. In some cases, this inflammation becomes excessive, causing collateral damage to the blood vessels and heart tissue. Dr. Scott Roberts, associate medical director for infection prevention at the Yale School of Medicine, explained that respiratory viruses increase cardiovascular risk in two main ways. The first is indirect, through inflammation that leads to stress on the cardiovascular system, blood clot formation, and the disruption of normal blood flow. The second is direct, where certain viruses can infect the heart muscle itself, causing myocarditis or other forms of heart tissue injury. “Unfortunately, many infections can do this,” Dr. Roberts said. “Generally, the more severe the viral illness, the greater the risk of cardiovascular complications.” Inflammation plays a central role in this relationship. Cytokine storms—excessive immune responses triggered during severe infections—can cause damage to arteries, making them more prone to plaque rupture, a leading cause of heart attacks and strokes. Moreover, persistent inflammation can lead to long-term scarring and stiffening of heart tissues, which impairs cardiovascular function even after recovery. Short-Term and Long-Term Effects The study’s findings show that the risk of heart attacks and strokes is especially high in the immediate aftermath of infection. Within weeks of contracting the flu or COVID-19, patients are more likely to experience cardiovascular events due to elevated inflammation and blood clotting activity. However, chronic viral infections—such as HIV, hepatitis C, and shingles—carry a different kind of danger: they can increase cardiovascular risk over the long term. These viruses often persist in the body for years, keeping the immune system in a constant state of activation. This prolonged inflammation gradually damages blood vessels and accelerates the development of atherosclerosis, a condition where fatty deposits build up inside arteries. Over time, this process can lead to coronary artery disease, stroke, and heart failure. Dr. Kawai noted that while acute viral infections pose immediate risks, chronic infections act more subtly, often causing years of silent damage before symptoms of cardiovascular disease become apparent. “It’s not just the patients who have underlying increased risk for cardiovascular disease that might be at greater risk,” he said. “Those who are younger adults, or people who might not necessarily have traditional risk factors, are also vulnerable after a viral infection.” Understanding the Mechanisms of Damage When viruses trigger inflammation, the immune system releases various proteins, including C-reactive protein (CRP), interleukin-6, and tumor necrosis factor-alpha. These compounds are known to damage the endothelium—the inner lining of blood vessels—making it easier for cholesterol and other substances to accumulate. In the case of COVID-19, researchers discovered that the virus can directly attack the ACE2 receptors in heart and lung tissues, leading to inflammation, microclot formation, and oxygen deprivation. This mechanism helps explain why patients recovering from COVID-19 often experience lingering symptoms such as chest pain, shortness of breath, and fatigue—collectively known as “long COVID.” Similarly, influenza viruses have been shown to destabilize arterial plaques, while shingles (caused by the reactivation of the varicella-zoster virus) can inflame blood vessels and increase stroke risk, particularly in older adults. Even less common infections such as cytomegalovirus, herpes simplex, and human papillomavirus (HPV) have been linked to cardiovascular complications, though further studies are needed to establish the exact biological mechanisms. Prevention Through Vaccination The evidence is increasingly clear that vaccination plays a crucial role in reducing cardiovascular risks associated with viral infections. Immunization helps prevent severe illness, reducing the chances of inflammatory responses that can damage the heart. Dr. Roberts explained that vaccines work by presenting the immune system with a harmless version of the virus or its components. This controlled exposure allows the body to build immunity without triggering the harmful inflammatory cascade seen in actual infections. “Vaccines for many of these viruses exist and generally lessen the risk of cardiovascular events after infection,” he said. Flu shots, COVID-19 vaccines, and shingles vaccines have all been proven to reduce not only infection rates but also the severity of illness, which translates to fewer cardiovascular complications. Health authorities continue to encourage adults, especially those with preexisting conditions like hypertension or diabetes, to stay up to date with recommended vaccinations. The Broader Public Health Perspective Cardiovascular disease remains the world’s leading cause of death, responsible for nearly 18 million fatalities each year. The new findings suggest that managing viral infections is a critical component of reducing this burden. Public health officials…